|
X-rays will reveal the joint narrowing and bone spurring but history often leads the physician to the appropriate diagnosis. Diagnosis is usually confirmed by history, examination and plain x-rays. Arthritis blood tests will also be negative. Blood tests (for blood inflammation) will prove negative because the inflammation is not in the blood but instead local in a joint. Swelling tends to occur with joint overuse or exertion and will subside with rest. It is possible to have a swollen joint at times but it is usually not long lasting. There is little inflammation in osteoarthritis compared to rheumatoid arthritis. Carrying extra body weight will accelerate the damage and symptoms of osteoarthritis. An old injury or smaller repetitive injuries can lead to a degenerative joint such as the knee or spine. It is possible to have more than one affected joint but there is no symmetry (as in rheumatoid arthritis). OA is a joint problem, not a systemic problem. OA does not affect the elbow or ankle unless there are other circumstances such as prior fracture or flat feet. Shoulder pain is usually NOT OA unless you have advanced impingement syndrome and have developed rotator cuff damage over the years. It can affect your neck and, to a lesser degree, the shoulders. It will also affect knees, hips (pain will be in the groin of the leg and inner aspect of the thigh, not on the side or buttock.) and spine. It does not cause harm to the knuckles of the hand (like rheumatoid arthritis). First, OA is most prevalent in the joints next to the fingernail (and toe) bed, the middle joints of the hand and the thumb base. Depending on the severity of the loss, OA can cause a variety of symptoms. OA can be present and painless for years until the loss becomes enough to warrant symptoms. Once this degeneration establishes, it can slowly (sometimes rapidly) cause more cartilage loss between the bones which leads to "bone-on-bone" and more pain. OA is a degeneration of the articular cartilage that covers the bone ends adjacent to each other. Osteoarthritis by definition means Osteo=bone, Arthro-joint and Itis=inflammation but these terms don't fully explain the problem. In the spine, terms can include degenerative disc disease, bulging disc, annular tearing, facet joint arthritis or arthrosis, degenerative spondylolisthesis or vertebral slipping, spinal canal or foraminal narrowing or spinal stenosis. Some patients don't realize they have arthritis because their doctor describes the problem as joint narrowing, never providing a specific diagnosis of osteoarthritis. Terms you may hear include joint deterioration, joint degeneration, joint narrowing, bone-on-bone, calcium deposits, bone spurs, joint diminishment or even "just" arthritis. 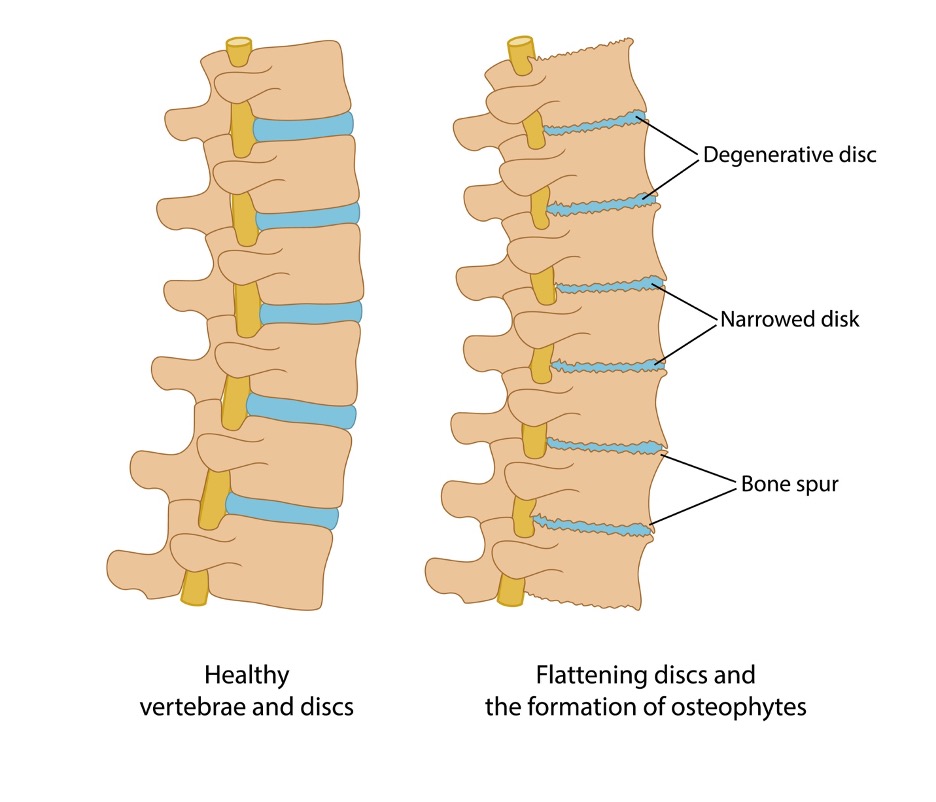
Physicians often use various terms to describe osteoarthritis. Osteoarthritis, also called degenerative arthritis or wear-and-tear arthritis, is the most common form of arthritis amongst more than 100 types. OSTEOARTHRITIS is a JOINT and CARTILAGE problem Let's take a few minutes to discuss the differences and hopefully, you will learn more about yourself and can determine if you are doing everything you can if you have arthritis or osteoporosis or osteopenia. Some of these conditions can be painful some are not and each has its own characteristics, signs and symptoms. Each condition is very different and requires different treatments. Frequently people speak of their condition and merge these problems together as they seek answers to their personal concerns. I ask, "Osteo-what?" As many of you know, there is osteoarthritis, osteopenia, osteoporosis, and others. During our seminars, I am often approached with questions.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
